Ozempic face:
- Kristine Ohkubo

- Mar 2
- 4 min read
A Medical Reality, Not an Insult: The Side Effect of GLP-1 Receptor Agonists
Nutrition is fundamentally intertwined with skin health, acting as the essential foundation for the skin's structure, repair mechanisms, and its ability to protect against various environmental damages. A balanced diet that is rich in antioxidants, particularly vitamins C and E, omega-3 fatty acids, and essential minerals such as zinc, plays a critical role in reducing inflammation, combating the signs of premature aging, promoting collagen production, and maintaining optimal skin hydration levels. These nutrients work synergistically to support a resilient skin barrier, which is crucial for defending against harmful UV radiation, pollution, and other skin conditions that may arise from external stressors.
Moreover, the role of diet in the development and management of skin disorders is well-established in medical literature, with numerous studies highlighting how nutritional deficiencies can serve as significant risk factors for various skin diseases. For instance, a lack of essential fatty acids can lead to dry, flaky skin, while insufficient intake of vitamins can result in conditions such as dermatitis or exacerbated acne. Imbalances in skin health can be triggered not only by deficiencies but also by excessive intake of certain nutrients, insufficient consumption of others, and exposure to hazardous ingredients found in some processed foods. Therefore, maintaining a well-rounded diet is not just beneficial but imperative for sustaining healthy skin and preventing potential disorders.

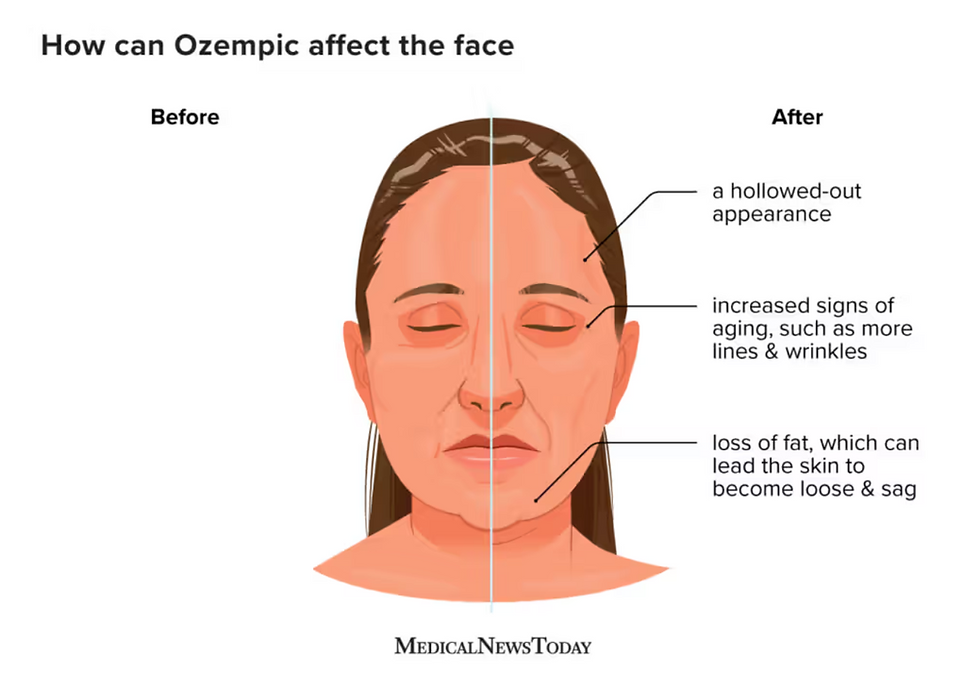
When it comes to the use of GLP-1 receptor agonists, such as semaglutide or tirzepatide, in individuals with a healthy body weight, these medications mimic the action of natural satiety hormones. They lead to delayed gastric emptying, increased insulin secretion, and suppressed appetite, which collectively contribute to significant weight loss. Patients often report a reduction in "food noise," which is the constant preoccupation with food, as well as lower blood pressure levels. However, it is crucial to recognize that such rapid weight loss can lead to potential nutritional deficiencies and gastrointestinal side effects, which can adversely affect overall health. Beyond the gastrointestinal discomforts, the phenomenon commonly referred to as "Ozempic face" can occur, characterized by sagging or sunken skin, muscle mass loss, and nutritional deficiencies that may arise from inadequate intake of essential nutrients during the weight loss process.

These medications, known by brand names such as Ozempic, Wegovy, Mounjaro, and Zepbound, have been approved by the FDA and are designed to drastically reduce appetite and hunger, often resulting in notable and rapid weight loss of approximately 15–20% of body weight in many patients. The mechanism by which these drugs operate involves slowing gastric emptying, which allows food to remain in the stomach for a longer duration, thereby enhancing feelings of fullness. However, this effect can also lead to chronic nausea, vomiting, or constipation in some individuals, which can further complicate their nutritional intake. Even in individuals who are otherwise healthy, these medications can lower blood glucose levels by stimulating insulin production while simultaneously suppressing glucagon, a hormone that raises blood sugar levels. This complex interaction underscores the necessity for careful monitoring of dietary intake and nutritional status for anyone undergoing treatment with GLP-1 receptor agonists, to mitigate the risk of adverse effects on skin health and overall well-being.

While designed primarily for the treatment of diabetes and obesity, the use of these medications in healthy individuals is largely considered off-label. This means that while healthcare providers may prescribe these drugs for purposes beyond their approved indications, such practices come with significant caveats. The long-term consequences of altering natural metabolic pathways and appetite-suppression mechanisms in individuals who do not have these conditions remain largely unknown and warrant careful consideration.
The medications in question are specifically formulated to target the physiological processes associated with type 2 diabetes and obesity, aiming to enhance insulin sensitivity, regulate blood sugar levels, and promote weight loss in individuals who are struggling with these chronic conditions. However, when these medications are administered to healthy individuals, the inherent risks may outweigh the benefits. For instance, the pharmacological effects that are beneficial in a diabetic or obese patient could lead to metabolic disruptions in someone with a normal metabolic profile.
The body’s natural metabolic and appetite-suppression pathways have evolved over time to maintain homeostasis. Interfering with these pathways through medication could lead to unforeseen consequences, such as hormonal imbalances or changes in energy expenditure that could predispose individuals to future health issues. For example, a healthy individual may experience a decrease in their natural appetite regulation, leading to overconsumption of food when not medicated, thus negating any short-term benefits of weight management.
It is crucial to emphasize that these medications are rigorously tested and approved by regulatory agencies for specific health conditions, such as type 2 diabetes and obesity, where the benefits have been demonstrated to outweigh the risks. In contrast, the application of these drugs in healthy individuals raises ethical and medical questions about the appropriateness of their use.

In summary, while the off-label use of diabetes and obesity medications in healthy individuals may appear appealing for weight management or metabolic enhancement, the unknown long-term consequences of altering natural metabolic and appetite-suppression pathways pose significant risks. It is essential for individuals to consult with healthcare professionals and consider the implications of such treatments, as the potential for unwanted or unintended health consequences is a serious concern that must be addressed.



Comments